Ultrasound (USG) guided nerve block is an evolving field that offers many potential benefits for surgery and anaesthesia. Nerves supplying the area of surgery are identified using ultrasound and drugs are deposited very close to the nerves which will provide pain relief and anaesthesia for surgery. This will ensure more definite and predictable action of the anaesthesia. The doses of drugs are also reduced. A complete body anaesthesia is avoided thereby reducing morbidity and mortality associated with anaesthesia significantly.
What is USG Guided Nerve Block ?
Ultrasound (USG) guided nerve block is an evolving field that offers many potential benefits for surgery and anaesthesia. Nerves supplying the area of surgery are identified using ultrasound and drugs are deposited very close to the nerves which will provide pain relief and anaesthesia for surgery. This will ensure more definite and predictable action of the anaesthesia. The doses of drugs are also reduced. A complete body anaesthesia is avoided thereby reducing morbidity and mortality associated with anaesthesia significantly.
What is the role of nerve blocks in anaesthesia ?
Nerve blocks can be used as main technique of anaesthesia or may be used as supplementary with other techniques depending on the surgery. When they are used as main technique of anaesthesia, the risks and complications of anaesthesia are reduced and recovery of the patient is much faster. When nerve blocks are used as supplementary to general anaesthesia, it provides excellent analgesia, reduces the preoperative anaesthetic requirements and postoperative analgesia requirements like opioids and therefore decreases complications like respiratory depression, drowsiness, nausea and vomiting.
What surgeries are performed under nerve blocks ?
Peripheral nerve blocks are commonly used for surgeries on the upper body and lower body. This may include the hand, wrist, arm, shoulder, breast, foot, ankle, knee, leg and hip.
How is USG-guided nerve block performed?
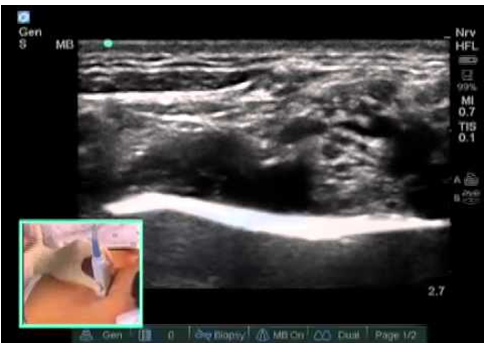
In the operation theatre, an IV (intravenous) will be inserted into one of your arms. ECG (Electrocardiogram), BP (blood pressure), SpO2 (oxygen saturation) will be monitored during the procedure. The area where the needle for the nerve block is inserted will be cleaned and local anaesthesia injected. Then anaesthesiologist will inject local anaesthetic medication around the nerves under direct visualization using ultrasound to make an area of your body numb. You may not be able to move this part of your body. The injection of local anaesthetic causes very little discomfort. The peripheral nerve block will be tested by an anaesthesia provider before surgery to make sure the desired area is numb.
What are the advantages of USG guided nerve blocks
When compared to general anaesthesia, peripheral nerve blocks cause less nausea and vomiting, less lingering drowsiness, no sore throat and often a faster discharge. Analgesia can be targeted specifically to the region of pain and provide relief for many hours, large volumes of local anaesthetic can be avoided. Often a nerve block will decrease your sensation to pain for a long time after surgery (6-24 hours). This provides better postoperative pain control.
To summarize, USG guided blocks are associated with less complications and provides higher patient satisfaction.
What are the limitations and complictions of nerve blocks ?
Complications with USG guided nerve blocks are very uncommon and rare. Complications of peripheral nerve blocks include infection, injury to blood vessels and the effects of local anaesthetic medication accidentally injected into a blood vessel (increased heart rate, seizures). Local anaesthetic toxicity is a theoretical possibility. It is uncommon for a block to cause injury to a nerve. In the rare event of an injury, complete recovery usually occurs in 6-8 weeks.
In the unusual case that a nerve block does not work completely, additional blocks, anaesthesia and/or pain medication may be easily supplemented.
Any preoperative fasting advice ?
6 hours of fasting for solids and 2 hrs for clear liquids is advised. This is because if the nerve block is not possible or fails, intravenous sedation or even general anaesthesia may be essential which requires fasting.
How is USG Guided nerve block for AV fistula surgery done ?
An arteriovenous fistula is the optimal form of vascular access in patients with end-stage renal failure requiring haemodialysis. A regional anaesthetic brachial plexus block results in vasodilatation and improved short- and long-term fistula flow compared to the infiltration of local anaesthetic alone.
Regional anaesthesia, such as a brachial plexus block (BPB), involves injection of LA around nerves to specifically block the motor and sensory nerves that supply the Upper limb, avoiding the need for general anaesthesia.
In the OR, an i.v line is placed in the free hand, and monitors attached. Using an ultrasound probe the nerves supplying the arm are blocked. Patients may have a mild electric shock like feeling in the hand and are instructed to inform anesthetist if it happens. This is an indication of the correct contact with nerve, and is not to be scared off. Over next 10-15 min, the operating hand starts becoming numb and heavy. After confirming adequate block, surgery is started. If block is not adequate, it will be supplemented with local anesthetic and I.V sedation if required.
What about postoperative care and precautions ?
Effect of nerve block may last for 6 – 8 hours depending on the concentration and volume of local anaesthetic used. So the limb can be heavy and numb even after completion of surgery. The power and sensation will gradually return to normal.
Reference
Vrushali C Ponde. An Illustrative Manual of Ultrasound Guided Regional Anaesthesia for Children & Adults. 2nd edition, 2013.
www.nysora.com